The second we moved to Nashville, it was clear that we were meant to be here. After almost a full year of medical struggles where it felt like we were always working to get on one doctor’s calendar or fighting the guidance of another, once we got to Nashville, everything sort of just started to fall into place. Even our trip to the DMV was a breeze!
We largely timed our moved around the availability of Sol’s new neurologist, who, after receiving a referral from our DC neurologist, was able to fit us into her schedule on October 1st. We packed up our home in DC on September 29th and travelled (me and the pups by car, Mike and Solly by plane) to Nashville on the 30th.
At our neuro appointment, we were referred to a physiatrist (in short, a movement doctor who will follow Solly for all of his childhood). This particular physiatrist typically has a 3 month waiting period to get on her schedule, but the day after our neuro appointment, I received a call from the physiatrist’s office saying they had a cancellation for the following week and would I like that appointment? Yes, please! The physiatrist then referred us for evaluations by physical, occupational, and speech therapies, as well as an appointment with another hard-to-book neuro ophthalmologist. We saw the neuro ophthalmologist only days later, thanks to another cancellation, and even though a friend warned that it’d likely be several months before we would be seen by the therapy department, we had all of our evals and were on a regular therapy schedule within two weeks of arriving in Nashville. We couldn’t have asked for a smoother transition!
Here’s a quick update on where we are on the medical side of things:
Neurology
Sol’s neurologist is an amazing woman. Our first appointment with her was so unlike our previous neurology appointments where everything seemed like a guessing game. (In our last neuro appointment in DC, the doctor said she was “nervous” about ever taking Sol off anti-seizure meds, even though he’s been seizure-free since the NICU. I’ve gotta say, hearing a doctor say she was nervous without any game plan didn’t give me a lot of confidence!) Our neuro reviewed Sol’s MRI and while she agreed that his damage is widespread and that we’ve got a lot of catching up to do, she wanted to move forward with an EEG to see if he was having any sort of seizure activity. She explained that though he has quite a bit of damage from his strokes, that doesn’t make him any more susceptible to seizures than any other stroke survivor. About 30% of pediatric stroke survivors will develop epilepsy, so there will always be a chance of recurrent seizures.
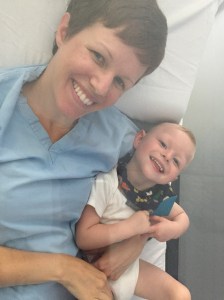
We went into Vanderbilt Children’s in early November for his repeat EEG. It stirred up so many horrible memories of our time in the NICU, where it seemed that he was always hooked up for an EEG which typically meant that we couldn’t hold him. Awful stuff. This time around, Sol was, at first, irritable when the tech affixed the sensors, but we were able to get his mind off of it with songs and toys. The EEG involved seeing how his brain responded to a series of blinking lights, how it was at rest, and how it reacted to falling asleep and waking up. Solly was a trooper and we were done with the EEG in about 45 minutes. Easy peasy! The best part was receiving a phone call from his neurologist 3 days later, saying he should zero seizure activity and his EEG looked great. His left side showed delayed responses, which, given the majority of his damage is there, makes sense and isn’t surprising. Our plan is to start weaning him off of Keppra (his current anti-seizure med) in the Spring was cold/flu season is over. Our next follow up with Solly’s neurologist is in January.

Falling asleep during the EEG

Happily done with the EEG
Physiatrist
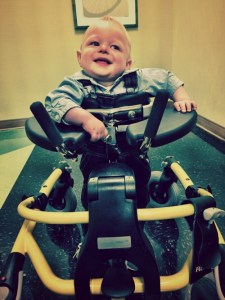
I was excited to meet our physiatrist. This is the one doctor I always wished we had in DC, but no one ever connected us with one. Basically, our physiatrist oversees all therapy and makes sure Sol gets exactly what he needs to support his development. Our first appointment with her consisted of a general evaluation of what he’s doing and how he’s moving, and what other doctors we needed to see now that we are in Nashville. Now that his physiatrist got us synced up with all therapists, the ophthalmologist, and a nutritionist, we are seeing her once again next week for an update. It’s obvious that this doctor has loads of experience and I really look forward to seeing her on a regular basis.
Neuro Ophthalmologist
Sol’s new neuro ophthalmologist took a look at Sol’s dilated eyes and told us what we already knew: the structure of his eyes is perfect, it’s possible he has a visual field cut (think: partial vision loss on one side), and he may also have strabismus. What’s nice is that he wants to wait and see how Sol’s vision develops before coming up with a solid plan of attack, so we don’t need to see him again for another year or two. I do, however, still have some concerns about how his vision is slowing down his gross motor development, so I may push to see another vision specialist sooner than that.
Nutritionist
The last of Sol’s specialists that will be following Solly is a nutritionist. You may recall that we’ve had quite a bit of trouble with Sol’s feeding over the last 6 – 8 months and this has (had!) been one of my biggest points of anxiety. Luckily, we’ve been having some major success with a feeding therapist (more on that soon), and as we’ve gotten better with eating, she and our physiatrist wanted Sol to see a nutritionist who could help us beef up Sol’s caloric intake. Our nutritionist is a super sweet lady. She walked me through Sol’s growth charts and said what we need to do is get him to gain some weight so his weight and height percentiles are more proportionate. (He’s about 25% for height and 2% or less for weight.) First of all, she took Sol off of Alimentum, thinking that he may not be eating as well because “it tastes like gasoline”, and put him on a high calorie version of Pediasure. Then, knowing that I’m a very goal oriented person, she gave me a target number of ounces he needs to consume every day as well as a daily calorie goal to fatten him up and make up for the weight he didn’t gain over the summer. Fortunately, after a couple of weeks, Sol has really taken to the Pediasure and has put on about 3 pounds since we’ve moved here. We check back in with her in February and I’m hopeful that Sol will continue to add the pounds so that appointment will be positive.
Solly has also been super busy at multiple weekly therapy appointments, but I’ll give a therapy update in our next post.
Thank you for keeping up with Sol’s adventures. We are so grateful for you!